Back decompressor that medicare pays for12/26/2023  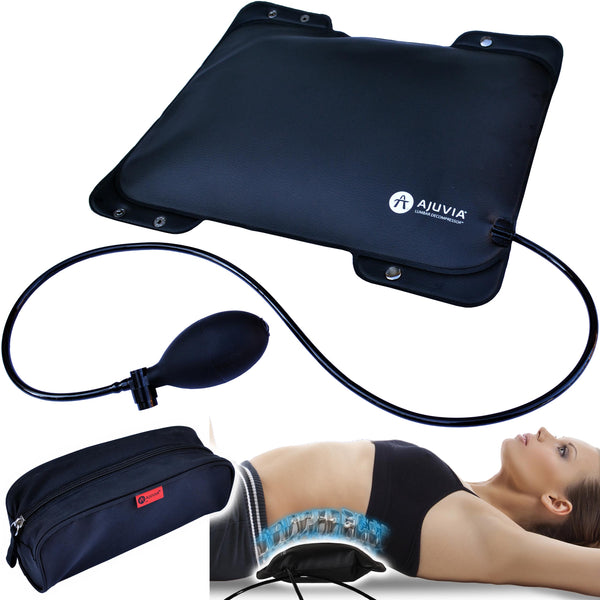
The bill has been passed by the House and is. At home if you are also receiving skilled home health or other skilled in-home services. In November 2021, the H.R.5376 Build Back Better Act was introduced to Congress, which would add hearing aids and hearing care to Medicare coverage. 
Now, let’s look high-level at some of the back pain treatment options Medicare may or may not cover. Medicare doesnt cover other services or tests a chiropractor orders, including X-rays, massage therapy, and acupuncture (unless the acupuncture is for the. Medicare: Only pays for long-term care if you require skilled services or rehabilitative care: In a nursing home for a maximum of 100 days, however, the average Medicare covered stay is much shorter (22 days). Again, that number could vary significantly. It is paramount you speak with your doctor and Medicare insurance provider before undergoing any treatment to properly understand what will and will not be covered, and what costs you may be fully or primarily responsible for. People who are eligible for Plan F enrollment can expect to pay a monthly premium between 150 and 400, with the average hovering around 230. Note: Just because the back pain treatment is covered, accompanying medical provisions such as anesthesia may not be if they’re not considered medically necessary. The treatment you receive to be done a certain way.You have tried less-invasive interventional treatments first (i.e., physical therapy) and they’ve been unsuccessful Vertebral axis decompression is NOT covered in accordance with the Centers for Medicare and Medicaid. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
